What is Chiari malformation?
Chiari malformation is thought to be the result of incomplete development at the lower rear of the skull that occurs during the embryonic period, which may be accompanied by complications such as syringomyelia and hydrocephalus. The most serious form is characterized by the herniation of a structure in the lower part of the cerebellum (the cerebellar tonsils) and the brainstem through the foramen magnum, so that some of the brain tissue extends into the spinal canal, causing it tos well and become compressed.
Chiari malformation type I
There are five types of Chiari malformations, but type I is by far the most common type. Chiari malformation type I (CM-I) consists of caudal displacement by more than 4 mm of the cerebellar tonsils below the foramen magnum. CM-I is not usually accompanied by the descent of the brainstem or fourth ventricle, nor associated with the presence of hydrocephalus; it is, nevertheless, typically associated with syringomyelia. Syringomyelia is a condition characterized by the formation of a fluid-filled cavity or cyst (syrinx) within the spinal cord that can slowly expand, causing progressive damage to the spinal cord and intracranial hypertension due to a rise in cerebrospinal fluid pressure.
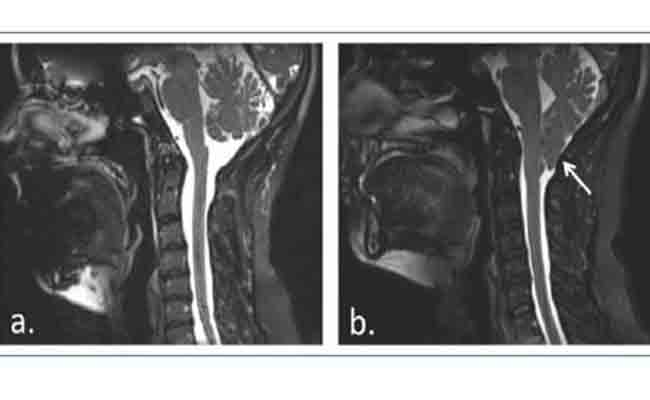
Symptoms of Chiari malformation
Symptoms can be numerous and varied, and can include motor, emotional, cognitive, perceptual and sensory deficits and dysautonomia. So as not to go into too much detail, I refer you to the bibliography where you can review all the possible symptoms and further information about Chiari (2,3).
Clinical case
A girl, diagnosed with Chiari malformation type I with syringomyelia, underwent surgery at the age of 12. After surgery, she sought specialized care at a neurorehabilitation center. When the neurorehabilitation program began, she was 13 years-old and in her second year of secondary school, with special needs for educational support.
The information collected during the patient’s interview and anamnesis is as follows:
- Achieves sitting position at 6-7 months-old.
- Ambulation at 18-20 months-old.
- Good language acquisition.
- Parental perceptions of clumsiness since she was born, in both gross and fine motor skills.
- Falls often and has an unsteady gait.
- Manual tasks such as drawing, writing, coloring, tying shoelaces, or putting toothpaste on the toothbrush are very difficult for her.
- Although she has always had difficulties at school, she has never repeated a year; however, she has needed support or accommodations for specific issues, such as giving her more time to do her daily homework and exams or taking multiple-choice exams, due to difficulties in writing and handwriting.
- Her family also reports that she is easily distracted and needs continuous supervision to carry out any task such as dressing, brushing her teeth or packing her backpack for school, and when she does, she is extremely slow.
- Does not show behavioral problems at home or at school that require special mention, beyond occasional angry outbursts or temper tantrums.
- However, parents report the presence of self-directed behaviors such as biting or scratching until hurting herself, though this only happens during the school year; on vacation, these behaviors subside.
- Has difficulties in forming and maintaining social relationships; sometimes shows an overly childish attitude and signs of immaturity that is not age-appropriate.
Motor assessment
Motor assessment revealed cerebellar signs and symptoms including disequilibrium, poor tandemgait, headtremor, truncal ataxia (swaying), fine tremor in distal parts of the body, dysmetria, and dystonic posture (worse on the left hand).
Neuropsychological evaluation
As for the neuropsychological evaluation, after undergoing a comprehensive battery of tests, the main findings were:
- Good orientation in space, time, and person.
- Regarding attentional processes, although sustained and selective attention were mildly impaired, impairment of alternating attention was significant,along with slower speed of information processing.
- With respect to executive functioning, she exhibited deficits in several subprocesses such as inhibitory control, cognitive flexibility, planning, and control and monitoring of goal-directed behavior. Difficulties were observed in problem solving, decision making and abstract reasoning
- She demonstrated adequateshort-term memory capacity, although this did not improve with the repetition of recall tasks, that is, her learning capacity was limited.
- Short- and long-term anterograde declarative memory deficits were observed, with difficulties in the consolidation and encoding of information, along with perseverationsin free recall and information recognition. This mnestic performance can be partly explained by attention and executive deficits.
- Concerning language, significant difficulty inreading comprehension, limited vocabulary, and deficits in verbal concept formation and verbal expression.
- Lastly, deficits in visuospatial skills, ideomotor, ideational and visuoconstructive apraxia, and difficulties with the execution of motor sequences and bimanual coordination were observed.
- In addition to the above, there were significant difficulties in the recognition of emotional expression, both her own and those of others, as well as a marked lack of empathy and social skills.
Improvement after one year of neuropsychological rehabilitation
One year after the beginning of neuropsychological rehabilitation conducted once a week, improvements have been observed in all cognitive functions, especially in memory and learning, in which she performs at an age-appropriate level. This improvement has reflected in her academic performance, gaining autonomy at home and performing better in homework and exams.
Can we explain the cognitive deficits in patients with cerebellar damage?
To make sense of this clinical case, can we explain the presence of cognitive deficits in patients with cerebellar damage? Of course. Although Chiari malformation is still considered to be a clinical entity that is typically characterized by the presence of motor deficits, numerous studies confirm what we already suspected about this malformation and about any pathology affecting the cerebellum: that is, that it will most probably present with cognitive deficits (4).
The available literature is clear: the cerebellum is involved in several processes and functions such as attention, learning, memory, executive function, visuospatial skills, language, social cognition, and affective and behavioral regulation. Below you will find a number of articles to read more about the functions the cerebellum contributes to (5,6,7,8,9,10,11,12,13,14,15,16,17,18).
Not only does the cerebellum play a role in many cognitive processes, but it is also part of functional brain networks which are the true foundation of cognition (19). As an example, here you have an image taken from a classic article by Dosenbach et al. 2008 (20), which shows in a very didactic way how the cerebellum fits in the functional brain networks involved in attentional and executive control.
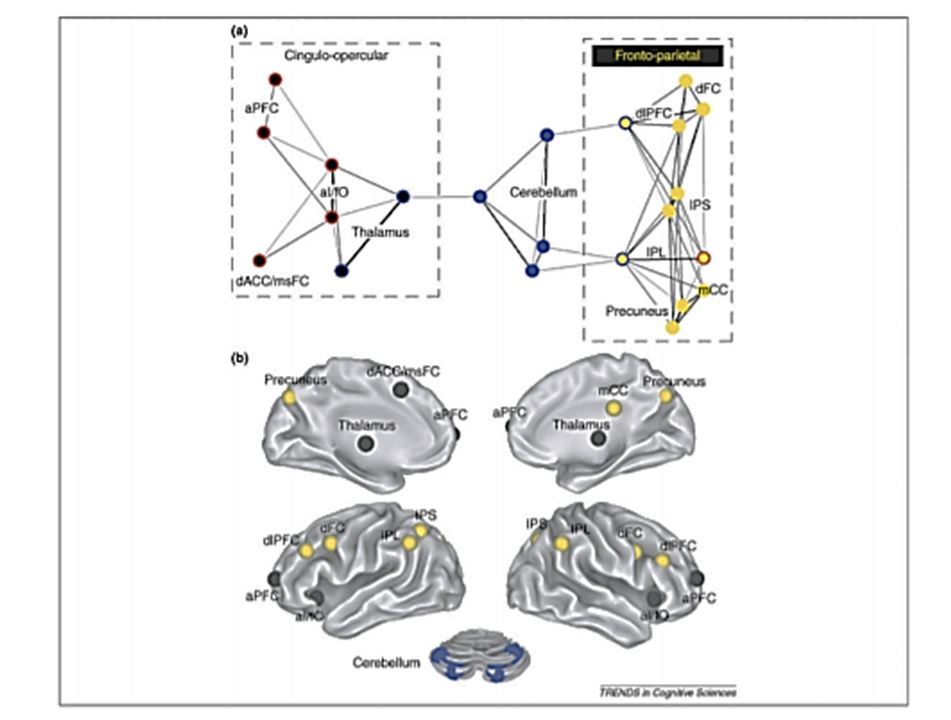
We must bear in mind that the prevailing view in neuroscience today—which should be part of our principles as neuropsychologists—is that the brain works based on widely distributed functional networks that are flexible and that dynamically adjust to the task at hand (21, 22), where damage to one of its components can trigger dysfunction of the entire network (23). Therefore, and in the light of all this data, we must abandon the traditional notion that made us expect specific deficits associated with focal brain damage, and inevitably head for a change of perspective in neuropsychological evaluation and rehabilitation (24).
Bibliography
- Federación Española de Malformación de Chiari y Patologías Asociadas. DOSSIER MC (MALFORMACION de CHIARI). Retrieved from: http://www.femacpa.com/index.asp?iden=11
- Documento de consenso. Malformaciones de la unión cráneo-cervical (Chiari tipo I y siringomielia). Retrieved from: http://www.sen.es/pdf/2010/Consenso_Chiari_2010.pdf
- Federación Española de Malformación de Chiari y Patologías Asociadas. Guía práctica. Retrieved from: http://www.femacpa.com/ficheros_noticias/boletin.compressed.pdf
- Rogers, J. M., Savage, G., & Stoodley, M. A. (2018). A Systematic Review of Cognition in Chiari I Malformation. Neuropsychology review, 1-12.
- Baillieux, H., De Smet, H. J., Paquier, P. F., De Deyn, P. P., &Mariën, P. (2008). Cerebellar neurocognition: insights into the bottom of the brain. Clinical neurology and neurosurgery, 110(8), 763-773.
- Kalron, A., Allali, G., & Achiron, A. (2018). Cerebellum and cognition in multiple sclerosis: the fall status matters. Journal of neurology, 265(4), 809-816.
- Baillieux, H., De Smet, H. J., Dobbeleir, A., Paquier, P. F., De Deyn, P. P., & Mariën, P. (2010). Cognitive and affective disturbances following focal cerebellar damage in adults: a neuropsychological and SPECT study. Cortex, 46(7), 869-879.
- Guell, X., Gabrieli, J. D., & Schmahmann, J. D. (2017). Embodied cognition and the cerebellum: perspectives from the dysmetria of thought and the universal cerebellar transform theories. Cortex.
- Van Overwalle, F., Baetens, K., Mariën, P., & Vandekerckhove, M. (2014). Social cognition and the cerebellum: a meta-analysis of over 350 fMRI studies. Neuroimage, 86, 554-572.
- Buckner, R. L. (2013). The cerebellum and cognitive function: 25 years of insight from anatomy and neuroimaging. Neuron, 80(3), 807-815.
- Sokolov, A. A., Miall, R. C., & Ivry, R. B. (2017). The cerebellum: adaptive prediction for movement and cognition. Trends in cognitive sciences, 21(5), 313-332.
- De Smet, H. J., Paquier, P., Verhoeven, J., & Mariën, P. (2013). The cerebellum: its role in language and related cognitive and affective functions. Brain and language, 127(3), 334-342.
- Timmann, D., Drepper, J., Frings, M., Maschke, M., Richter, S., Gerwig, M. E. E. A., & Kolb, F. P. (2010). The human cerebellum contributes to motor, emotional and cognitive associative learning. A review. Cortex, 46(7), 845-857.
- Leggio, M. G., Chiricozzi, F. R., Clausi, S., Tedesco, A. M., & Molinari, M. (2011). The neuropsychological profile of cerebellar damage: the sequencing hypothesis. cortex, 47(1), 137-144.
- Peterburs, J., & Desmond, J. E. (2016). The role of the human cerebellum in performance monitoring. Currentopinion in neurobiology, 40, 38-44.
- Tirapu Ustárroz, J., Luna Lario, P., Iglesias Fernández, M. D., & Hernáez Goñi, P. (2011). Contribución del cerebelo a los procesos cognitivos: avances actuales. Rev Neurol, 301-315.
- Hernáez-Goñi, P., Tirapu-Ustárroz, J., Iglesias-Fernández, L., & Luna-Lario, P. (2010). Participación del cerebelo en la regulación del afecto, la emoción y la conducta. Revista de neurología, 51(10), 597-609.
- Van Overwalle, F., & Mariën, P. (2016). Functional connectivity between the cerebrum and cerebellum in social cognition: a multi-study analysis. NeuroImage, 124, 248-255.
- Maestú, F., Quesney-Molina, F., Ortiz-Alonso, T., Campo, P., Fernández-Lucas, A., & Amo, C. (2003). Cognición y redes neurales: una nueva perspectiva desde la neuroimagen funcional. Rev Neurol, 37(10), 962-6.
- Dosenbach, N. U., Fair, D. A., Cohen, A. L., Schlaggar, B. L., & Petersen, S. E. (2008). A dual-networks architecture of top-down control. Trends in cognitive sciences, 12(3), 99-105.
- Pessoa, L. (2017). A network model of the emotional brain. Trends in cognitive sciences, 21(5), 357-371.
- van den Heuvel, M. P., & Pol, H. E. H. (2011). Exploración de la red cerebral: una revisión de la conectividad funcional en la RMf en estado de reposo. Psiquiatría biológica, 18(1), 28-41.
- Gratton, C., Nomura, E. M., Pérez, F., & D’Esposito, M. (2012). Focal brain lesions to critical locations cause widespread disruption of the modular organization of the brain. Journal of cognitive neuroscience, 24(6), 1275-1285.
- Price, C. J. (2018). The Evolution of Cognitive Models: From Neuropsychology to Neuroimaging and back. Cortex.
 Borderline personality disorder: a personal story
Borderline personality disorder: a personal story

Leave a Reply